There are two ways ultrasound can be used to assess a woman’s fertility:
• Transabdominal Ultrasound Scan (a scan through the lower belly)
• Transvaginal Ultrasound Scan (a scan from inside the vagina)
Transabdominal Ultrasound Scan
The transabdominal scan is likely to be the first fertility ultrasound you are sent for. It is performed on your lower abdomen (lower belly).
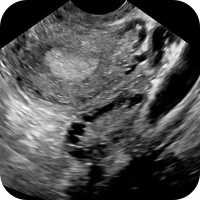
You will be given a hospital gown to put on and asked to take off your trousers (or skirt) and pants behind a privacy screen. You will then be asked to lay on a couch and your modesty will be protected by the judicious application of a large paper towel. The sonographer (the person doing the scan) will apply gel to your tummy. This gel is a conducting gel which improves the image quality of the scan. Onto this gel, the sonographer will then hold an ultrasound transducer, which is a handheld device connected to the ultrasound machine. This transducer sends the ultrasound waves through you and picks up the returning waves. This enables the ultrasound machine to create the grainy black and white picture of your insides.
The whole process takes between 5 and 10 minutes and once completed, you will be allowed to put your clothes back on and use the toilet to empty that full bladder.
It is unlikely the sonographer will discuss what they are seeing while they are performing the scan or even afterwards. You’ll have to wait until you see your doctor next for the results, as the scan findings will be sent to them to discuss with you.
Transabdominal Ultrasound Preparation
For this ultrasound scan you will need a full bladder. So either be prepared to travel to the appointment with a full bladder, or arrive early and drink a lot of water when you get there.
Sometimes the examination room can be a little on the cold side and you will need to remove your trousers and pants. If you feel the cold (like I do), you may want to consider wearing extra thick, long socks. Usually you will be allowed to keep your top on, but rolled up, so make sure you can easily roll it up. The gel that is put on your tummy isn’t always warmed up before use, so prepare for this to be cold too.
Why Do You Have to Have a Full Bladder for a Transabdominal Ultrasound?
This is because a full bladder pushes your intestines aside. Ultrasound does not travel very well through the contents of your intestines, especially through intestinal gas. However, ultrasound travels very well through the liquid in your bladder and because of this, you will get a better picture on the ultrasound.
Sometimes, even with a full bladder, it is not possible to fully see the ovaries and uterus in a transabdominal ultrasound. This is because even with a full bladder, the bowel can still be in the way and the bowel gas obscures the pictures. If this is the case, the sonographer may proceed (with your consent) to a transvaginal ultrasound. This will give them better pictures and mean that you don’t have to go back for another scan at a later date.
Transvaginal Ultrasound Scan
This type of scan produces a higher quality image than the transabdominal ultrasound. However, it is more invasive as it requires the ultrasound transducer to be inserted into the vagina rather than just rested on the abdomen. On the plus side, you are not required to have a full bladder for this ultrasound.
Your doctor will send you for a transvaginal ultrasound scan if there is anything from the transabdominal scan they want to get a more detailed look at. Though it is worth noting that some doctors will skip the transabdominal scan altogether and recommend you go straight for a transvaginal scan.
Like a transabdominal ultrasound, you will need to remove your trousers and pants, and will be given a gown to wear. However, transvaginal ultrasounds require you to put your feet in stirrups, instead of just lying on a bed.
If you have previously had a transabdominal ultrasound, do not worry that they will use the same size ultrasound transducer. The transducer used for a transvaginal ultrasound is small and thin. This transducer is first covered with a condom like sheath, which is then lubricated with gel. If you have a latex allergy, make sure you tell the sonographer, as they will then use a non-latex sheath.
For the scan, the sonographer will insert the transducer about five centimetres into your vagina. They will then need to move it around very slightly in order to get images of your reproductive organs. The sonographer may also ask you to press on your abdomen, this is so that they can a better image of your ovaries.
Like the transabdominal ultrasound, the sonographer is unlikely to discuss the results of the scan with you. However, you can ask to see the images of yourself as they are being taken. These aren’t easy to interpret, but from personal experience, it helped to distract me from what was going on down below.
Transvaginal Ultrasound Preparation
Unlike the transabdominal ultrasound, the transvaginal ultrasound does not require you to have a full bladder. However, you may want to consider wearing the thick socks and a top that easily rolls up to the exam in order to remain warm.
Transvaginal Ultrasound Pain
The transvaginal ultrasound maybe a little uncomfortable, but it should not be painful. In fact, I have heard more complaints about the use of stirrups than I have heard about the insertion of the transducer. If you should experience any pain during the procedure (and you really shouldn’t), immediately let the sonographer know as this is not normal.
The Initial Fertility Ultrasound Scan
The initial scan is the one that all women who have seen their doctor will be sent for. It looks at the general health of your reproductive organs, as well as looking for specific tell-tail signs that something may be wrong. I have listed the specific signs they are looking for below, broken down by the part of your reproductive system they are found in:
Uterus Ultrasound Scan
Your uterus (the womb), is the place within your body that the baby develops. A fertility ultrasound scan will check for the following:
- The uterus lining (the endometrium) is the correct thickness. Too thin and embryos are less likely to implant. Too thick and there may be a hormonal problem. The thickness of this lining changes throughout your cycle. As you could be called in for your initial ultrasound scan at any point, it is helpful to know where you are at in your cycle so they can work out if the lining is at the correct thickness for that time or not
- There are no large fibroids. These are balls of muscle tissue that if big enough, can change the shape of the uterus cavity and cause embryo implantation problems or simply not allow enough room for the foetus to grow
- That the uterus is shaped normally. An abnormally shaped uterus can hamper embryo implantation or not provide enough room for the foetus to grow. Examples conditions are the bicornuate uterus (also known as a “Heart Shaped” uterus) or the uterine septum where the uterus is partitioned
- That you don’t have any endometrial or cervical polyps. These are growths from the wall of the uterus or cervix that extend into the uterine cavity and prevent embryo implantation much like the contraceptive coil
- Blood flow around the uterus and to the uterus lining. A good blood supply is needed to transport oxygen and nutrients, and allow the uterus lining to develop properly during the cycle. This is not currently a standard test carried out by national health services, but is often carried out in conjunction with assessment of the ovary health as part of a paid private patient procedure. The method used to measure blood flow is called Doppler imaging (it uses the Doppler effect, where sound wave frequency changes as the object it is coming from moves relative to the observer of the sound waves. This can be used to measure the speed of red blood cells moving along blood vessels)
Ovaries Ultrasound Scan
Your ovaries are where your eggs are stored. Each menstrual cycle, one or more eggs will develop within the ovary into a follicle and once matured, are released for fertilisation. As well as checking you have ovaries and they are creating egg follicles, the fertility ultrasound scan will also look for:
- Multiple cysts on the ovaries. This could indicate you have Polycystic Ovary Syndrome (PCOS), which a further blood test would be able to confirm
- Cysts caused by Endometriosis. This condition is where the uterus lining (the endometrium) is found outside the uterus. As well as causing cysts, endometriosis on the ovaries can interfere with the maturation and release of eggs
- Other cysts on the ovaries. If large these can cause pain, interfere with the work of the ovaries and affect the release of eggs.
- Antral follicles, also as known as resting follicles, these are small follicles that are waiting their turn to mature for release. A count of these are used to estimate a woman’s fertility potential. This is not a common procedure for a national health service and is likely to only be done as part of a paid private patient procedure
- Blood flow around the ovaries. This is an additional test used to assess ovary health, as a good flow of blood to the ovary ensures it is well supplied with oxygen and nutrients. This is another form of Doppler imaging and is usually only performed in a private patient fertility setting, where it is used in conjunction with an antral follicle assessment
Fallopian Tube Ultrasound Scan
The fallopian tubes connect your ovaries to your uterus (you have one tube for each ovary). The fertility ultrasound scan is looking for:
- Any swelling which may indicate a blockage to the tube. If this is detected, a Hysterosalpingogram (HSG) can confirm if there is a blockage or not
- Signs of Endometriosis. While it is not easy to see actual endometriosis on the fallopian tubes, it can leave tell-tail signs like scarring or kinking of the tubes. Endometriosis in the fallopian tubes can either block the tubes or interfere with the cilia (little hair like structures that move in rhythmic waves) that aid transportation of the egg along the tube
- Scarring. While this could be a sign of endometriosis, it may also be caused by an infection. Scarring of the fallopian tubes can block the tube or interfere with the cilia movement
Ultrasound Scans During Fertility Treatment
Ultrasound scans are an essential part of many fertility treatment plans. Generically speaking, they are used to monitor your cycle, check how treatment is proceeding, and when to retrieve and implant eggs. Precisely what they are used for and how often you need to go for them will depend on your personal treatment plan. However, to give you an idea of what they might be used for, below are some common uses during fertility treatment:
Monitoring the effect of fertility drugs
To do this, they look at the endometrial (uterus lining) development, egg follicle growth and ovulation. If things are not going according to plan, they may modify the amounts of the drugs you are given and even change the drugs themselves.
Timing Egg Retrieval and Embryo Implantation
By monitoring egg follicle growth, they can work out the best time to remove your eggs for treatments like IVF. By monitoring your endometrial development, they can work out the best time to put your fertilised eggs back in so that they have the best chance of implanting into your endometrium.
During Surgical Procedures
Ultrasound is used to guide the egg retrieval needle to the mature egg follicles in the ovaries.
How Do Ultrasound Scans Work?
Ultrasound machines have been around since the 1950s and use a form of echolocation (producing a sound and locating things from the echo coming back from them). They work a bit like the sonar used by bats and dolphins.
Ultrasound machines generate high-frequency ultrasound pulses that are transmitted through your body using a transducer (the wand-like bit that the sonographer holds against you). When the ultrasound pulses hit different densities of tissues and bone, some of the pulses get reflected back to the transducer. The transducer picks up these return pulses and they get relayed to the ultrasound machine. The machine then calculates the amount of pulses that have returned and how long it has taken for them to return. These calculations are then used to interpret what your insides look like. This happens in real time, with the image being displayed on a monitor. Then by moving the transducer around, different parts and angles of your insides can be seen.
Ultrasound scans do have limitations though. They have difficulty seeing through bone because it is so dense. They also have difficulty seeing through air and gas, because it is not dense enough. The latter is the reason you have to have a full bladder for a transabdominal scan; gas in the intestines makes scanning difficult and a full bladder pushes the intestines out the way of the scan.
The whole process is very safe and there are no known risks associated with it.
Fertility Ultrasound Scan Final Thoughts
If you decide to use a private fertility clinic for treatment, it is worth noting that you may require several visits for fertility ultrasound scans. If your clinic is a long distance away, the long journeys to and from the clinic could prove problematic (especially if your clinic is abroad). So remember to ask prospective fertility clinics if you can access ultrasound facilities more local to you.
For more information on the types of tests your doctor will send you for, check out: Fertility Tests.
Links to Popular Related Pages